-
-
Featured Care Areas


Source: Shutterstock
Caring for Your Child with Eczema
Last updated: Thursday, January 30, 2020 | 8 min reading time
While eczema is a common skin condition which can affect people of all ages, it can be particularly tricky when your child is diagnosed with eczema.
As the parent or caregiver of a child with eczema, you know the heartache and frustration this brings, not just for the child but for you in watching them suffer and feeling helpless to do anything to alleviate their discomfort.
The itching at night, restless sleep, constant scratching, irritability, discomfort, and worries about your child being stigmatised at school all add up and can take their toll.
In this article, we share some approaches you can take to help control your child's eczema and prepare you both to deal with living with eczema better.
How parents can help manage and care for your child's eczema
Pick a gentle soap-free cleanser for bathing
Pick a gentle cleanser for your child that is fragrance-free and non-soap based so as to minimise aggravation to the skin when cleansing. Read the labels for cleansers to look for those specifically designed for eczema or ask your doctor to recommend a trusted cleanser. Avoid prolonged baths or soaking in the tub. Avoid products with fragrances, parabens and multiple additives. If the skin is broken, bathing your child in bath oils can bring much-needed relief.
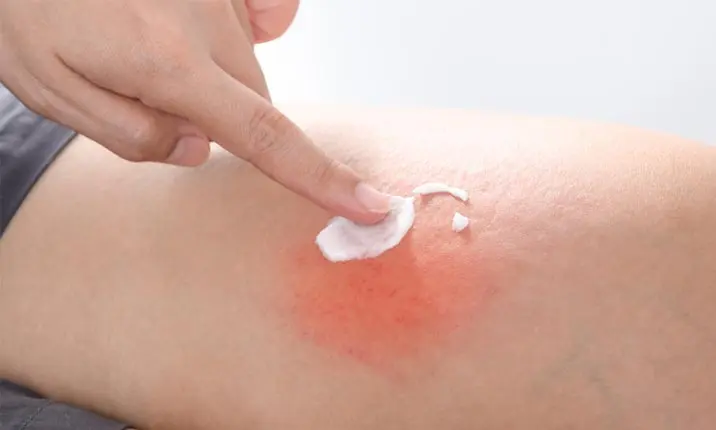
Moisturise the skin liberally
The key to controlling eczema is keeping the skin fully moisturised. This means liberally applying fragrance-free and additive-free moisturiser designed to treat eczema. Apply as needed, at least 2 times a day. Moisturising should be done immediately after baths as baths are drying to the skin. Another good time to moisturise is right before bedtime so that the skin is kept moist and itching can be reduced during sleep.
If you are not sure if you are using enough, a normal tube should last no more than 2 weeks. Experiment with different brands until you find one your child likes the feel of.
Avoid irritants
Products with perfumes, fragrances, powders and additives may further irritate your child's skin so read all labels carefully to avoid putting such products on your child’s skin.
Dealing with skin infections
Skin infections caused by Staphylococcus aureus are common in children with poorly controlled eczema. This is because scratching breaks the skin barrier and allows the bacteria to enter sometimes even into the bloodstream. In some cases, your child may require a short course of antibiotics.
To prevent such skin infections, use antiseptic washes during periods of eczema flare-up. Your doctor may prescribe washes such as Octenisan, chlorhexidine, zinc washes etc. In some countries, people may use bleach baths as well. These washes help to reduce the amount of bacteria on the skin and help reduce the inflammation. As these washes tend to dry the skin, take extra care to apply moisturiser liberally after as well.
A more "fun" antiseptic treatment for your child is a session in the swimming pool. The chorine in the water helps to keep the skin clean. After swimming, wash off excess chlorine at the poolside and moisturise liberally. Chlorine is also drying, so have your child take a shower immediately afterwards and moisturise the skin liberally.
When steroids are needed
You should aim to control your child's eczema so you don't have to depend on steroids. However, sometimes this can't be helped and your doctor may recommend a short course of steroid creams to bring the condition under control. As prolonged or incorrect use of these creams can cause the skin to redden and thin, always follow the doctor's prescription and guidelines.
Wet wrap technique for tackling severe eczema
If your child experiences intense eczema flares with severe itch or pain, your doctor may suggest wet wrap therapy. Wet-wrap techniques are reported to be a safe and effective treatment option in children with severe eczema in whom other treatments have failed.
What is wet wrap therapy?
Wet wraps are bandaging techniques that rehydrate and calm the skin. Wet wraps reduce redness and inflammation and promotes skin healing. Wet wraps also help to reduce the itch and serves as an effective barrier to scratching. This promotes more restful sleep in children with eczema.
Two sets of bandages should be measured and cut before bathing. The skin should be well moisturised - apply moisturiser to the whole body and face in a downward motion. Dip the tubular bandage in lukewarm water, and remove the excess water. Apply the warm, damp bandage onto your child's skin. Next, cover the wet bandages with dry tubular bandages. Lastly, dress your child in cotton, firm fitting pyjamas.
Points to remember when using wet wraps
Wet wraps should be preferably used at night; however, they can also be used during the day if the eczema is severe. Do not leave the wraps to dry as they can irritate the skin and make it dry and itchy. To avoid this situation, spray water onto the dry tubular bandages frequently every few hours and also before removing the bandages.
Wet wraps can be used for a maximum duration of one week. It is recommended to consult your doctor after that.
Choosing suitable clothing
Choose cotton or cotton-blend clothing for your child. Avoid synthetic materials as these do not allow the skin to breathe and will cause sweating and irritation.
Launder new clothing before use to reduce formaldehyde and chemical contents added during the manufacturing process. Use mild detergents as indicated on the packaging. Pick liquid detergents over powdwhers and use an extra rinse cycle on the washing machine to remove as much of the detergent from the clothing as possible.
Food and other allergens that can trigger eczema flare-ups
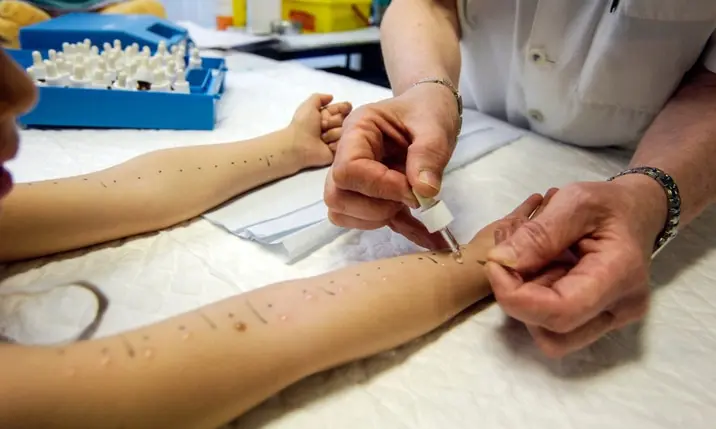
Up to one third of infants and toddlers have some form of food allergy which can trigger an eczema flare-up, but this is less likely to happen as the child grows older. If you suspect a food allergy, it is important to consult an allergy specialist who may do a skin prick test or blood test if there is a clinical suspicion of food allergy. Avoid removing multiple foods from your child's diet as most aren't causing true allergies. By eliminating multiple foods from your child's diet, you risk affecting their nutrition and they may end up not getting a balanced diet.
In young babies, it is not advised to apply creams or lotions with food grade ingredients such as oat and coconut etc. to the skin as there is increasing evidence that topical application of food grade ingredients prior to oral dietary exposure could lead to the development of true food allergies. Conversely, earlier oral introduction of foods by 4 – 6 months of age may help reduce the development of food allergies in babies with eczema. Your allergist will be able to help guide you with this weaning process.
In older children, house dust mite sensitivities may trigger eczema. Take precautions to reduce dust mite load at home by keeping the environment clean. Don't place carpets, rugs and stuffed toys in your child's room and around the house. Use anti-dust mite covers or simply wash bedding in hot water (at least 60 degrees) once a fortnight or more. Since dust mites thrive in indoor environments, allow your child to have an active outdoor lifestyle as this will also minimise their exposure to dust mites.
Vitamin D and E
There is some evidence that vitamin D and vitamin E supplementation (at 1000IU/day and 400IU/day respectively) in children with eczema may help reduce the extent and severity of eczema. These vitamins have been shown to have anti-inflammatory properties and may have positive effects on the skin barrier integrity in eczema. Children who are vitamin D deficient are at risk of developing more severe eczema.
Managing school and sports activities
Eczema should not impact your child's enjoyment of school and they should not be singled out for special treatment. The only concession should be in sports activities, which your child should be fully encouraged to take part in. Just be sure that the teachers know that your child should take a shower or use a moist towel to wipe off sweat immediately afterwards as this can irritate the skin. Make the teachers aware of the needed cleaning and moisturising routine and that your child should be allowed to change into fresh dry clothes.
If your child's skin condition gives rise to any bullying or teasing, do bring it up to the teacher, who is experienced at handling the situation and educating the class.
Protecting the skin during outings
Arrange outings for cooler and less humid times of the day, where you can, to minimise sweating.
Use non-sensitising sunscreen such as those formulated for the face, which are usually better tolerated in children with eczema. You may want to do a 'patch test' with new products on a small area of skin to check if they irritate your child's skin.
Planning overseas trips
As sweating can irritate eczema-inflamed skin, consider more temperate climates for your holidays away. If you do travel to tropical countries, allow for frequent breaks to wipe down sweat and get a fresh change of clothing.
Ensure that you pack in your child's bag washes and sufficient moisturiser to last the trip, as his specific brand may not be available overseas. Bring a travel-sized tube of moisturiser for the plane and apply it frequently during long flights to keep the skin moist.
Follow your eczema action plan from your doctor in case of flare-ups overseas, and seek medical attention if your child's skin continues to worsen despite the steps on the action plan. The action plan may include instructions for a short course of gentle topical steroids in the event of a moderate or severe flare-up.
Boosting your child's self-esteem
Boost your child's self-esteem by constantly reinforcing strengths and helping them realise that they should not be judged by their skin condition or any other physical appearance. Work with your child to build acceptable strategies to deal with teasing or bullying from others. It is important not to further stigmatise eczema by curbing your child’s activities or preventing them from joining in with their peers.
Psychological stress is known to play a part in flare-ups of eczema. Keep an eye out for any stressors at home or school that can have an impact on your child's mental health and act early to help your child cope. If your child shows any signs of persistent low mood or depression, flag this up to your doctor. Some children may benefit from seeing a specialist such as a psychologist or play therapist to help them deal with these issues better.
Although lifestyle changes can help better control eczema, it's important that parents not make too many changes at once. Consult your paediatrician before making any significant changes to your lifestyle.
Learn how you can recognise and manage your child's eczema symptoms.
Mansour NO, et al. The impact of vitamin D supplementation as an adjuvant therapy on clinical outcomes in patients with severe atopic dermatitis: A randomized controlled trial. (2020, November 3) Retrieved October 25, 2021, from https://bpspubs.onlinelibrary.wiley.com/doi/10.1002/prp2.679