-
-
Khu vực chăm sóc và điều trị


Nguồn: Shutterstock
Nhận biết sự khác biệt giữa u nang buồng trứng và u xơ tử cung
Cập nhật lần cuối: 21 Tháng Ba 2022 | 4 phút - Thời gian đọc
U xơ và u nang là những bất thường cấu trúc rất phổ biến của hệ sinh sản nữ và thường ảnh hưởng đến phụ nữ trong độ tuổi sinh đẻ.
U xơ và u nang ảnh hưởng đến các cấu trúc khác nhau trong hệ thống sinh sản của phụ nữ. Tuy nhiên, cả hai đều có thể biểu hiện với các triệu chứng tương tự, chẳng hạn như đau vùng chậu và chảy máu tử cung bất thường. Cũng có khả năng cả hai tình trạng này đều có thể ảnh hưởng đến khả năng sinh sản.
U xơ ảnh hưởng đến tử cung trong khi u nang xảy ra ở buồng trứng. Phương pháp điều trị phụ thuộc vào các triệu chứng, kế hoạch sinh con và có thể ở dạng không phẫu thuật cũng như can thiệp phẫu thuật. Cả u xơ và u nang đều được chẩn đoán bằng siêu âm.
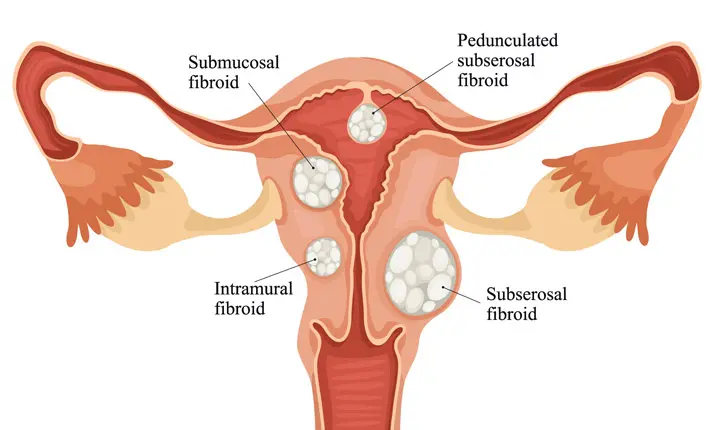
U xơ tử cung là gì?
U xơ tử cung là sự phát triển khối cơ bên trong thành tử cung không gây ung thư. Chúng có thể có đường kính lên tới vài cm nhưng thường không bị phát hiện vì có thể không gây ra bất kỳ triệu chứng rõ ràng nào. U xơ tử cung rất phổ biến và khoảng 50% phụ nữ sẽ mắc u xơ khi họ bước sang tuổi 50. Những u xơ này thường được phát hiện khi họ đi khám phụ khoa định kỳ. May mắn thay, hầu hết phụ nữ bị u xơ tử cung có kích thước nhỏ và hiếm khi có triệu chứng. Trung bình, chỉ có 25% phụ nữ gặp phải các triệu chứng.
Các triệu chứng của u xơ tử cung là gì?
Bạn có thể bị u xơ tử cung nếu gặp các triệu chứng sau:
- Giai đoạn nặng nề và đau đớn;
- Chảy máu tử cung bất thường;
- Co thắt vùng bụng và vùng chậu;
- Đau dưới thắt lưng;
- Đau hoặc áp lực khi quan hệ;
- Đi tiểu thường xuyên Hoặc khó khăn.
Khi nghi ngờ, hãy tham khảo ý kiến bác sĩ phụ khoa vì u xơ tử cung có thể làm phức tạp quá trình mang thai và có thể dẫn đến sẩy thai và/hoặc vô sinh.
Nguyên nhân của u xơ tử cung là gì?
Nguyên nhân chính xác của u xơ tử cung vẫn chưa được biết, nhưng chúng có liên quan đến:
- Estrogen và progesterone là những hormone kích thích sự phát triển của niêm mạc tử cung trong mỗi chu kỳ kinh nguyệt. u xơ chứa nhiều thụ thể hormone này hơn các cơ khác trong tử cung và việc Giảm sản xuất hormone trong thời kỳ mãn kinh đôi khi khiến u xơ Co lại.
- mang thai, làm tăng sản xuất Estrogen và progesterone.
- tiền sử gia đình mắc bệnh u xơ, đặc biệt là trong số những người Thân như mẹ Hoặc chị gái của bạn.
Các yếu tố khác có thể làm tăng nguy cơ phát triển u xơ tử cung là:
- Béo phì;
- Chế độ ăn nhiều thịt đỏ và ít rau, trái cây và các sản phẩm từ sữa;
- Tiêu thụ rượu;
- Thiếu vitamin D;
- bắt đầu có kinh nguyệt sớm.
Nhìn chung, tiền sử gia đình mắc bệnh u xơ tử cung có thể cho thấy nguy cơ mắc bệnh này, nhưng duy trì lối sống lành mạnh và kiểm soát cân nặng có thể làm giảm nguy cơ phát triển u xơ tử cung ở phụ nữ.
U xơ tử cung được điều trị như thế nào?
Kế hoạch điều trị u xơ tử cung sẽ phụ thuộc vào mức độ ảnh hưởng của các triệu chứng đến cuộc sống hàng ngày của bạn, khả năng hoạt động bình thường của cơ thể và liệu bạn có dự định sinh con hay không.
U xơ tử cung có thể ảnh hưởng đến khả năng sinh sản của bạn
Trong khi nhiều phụ nữ bị u xơ tử cung không phải đối mặt với các vấn đề về sinh sản và mang thai thành công thì một số u xơ tử cung có thể gây viêm niêm mạc tử cung và thay đổi môi trường nội tiết tố cục bộ, ảnh hưởng đến quá trình làm tổ của phôi.
Nếu u xơ quá lớn, nó có thể dẫn đến thay đổi hình dạng cổ tử cung, ảnh hưởng đến số lượng tinh trùng có thể xâm nhập vào tử cung hoặc cản trở sự di chuyển của tinh trùng hoặc phôi. U xơ tử cung cũng có thể làm tắc ống dẫn trứng, gây khó khăn cho việc thụ thai.
Thuốc
Bác sĩ phụ khoa của bạn có thể áp dụng phương pháp theo dõi và chờ đợi để xem liệu thuốc có thể làm giảm các triệu chứng của bạn hay không.
Thuốc nội tiết có thể được kê toa để điều chỉnh chu kỳ kinh nguyệt của bạn, giảm đau và chảy máu. Thuốc cũng có thể ngăn chặn sự phát triển của u xơ.
Điều trị u xơ tử cung nếu bạn đang cố gắng thụ thai
Nếu bạn đang có kế hoạch thụ thai, thuốc có thể được kê đơn để giúp thu nhỏ khối u xơ hoặc một thủ thuật được gọi là phẫu thuật cắt bỏ u xơ có thể được khuyến nghị để loại bỏ chúng.
Nó cũng có thể giúp thực hiện một số thay đổi trong lối sống như tránh các thực phẩm có hàm lượng calo cao, giảm lượng thịt ăn vào, tăng lượng rau xanh và cá như cá ngừ hoặc cá hồi. Giảm cân và kiểm soát mức độ căng thẳng của bạn cũng có thể hữu ích.
Phẫu thuật cắt bỏ u xơ để loại bỏ u xơ
Phẫu thuật cắt bỏ u xơ là một thủ thuật để loại bỏ u xơ khỏi tử cung mà không cần cắt bỏ toàn bộ tử cung.
Điều này giúp phụ nữ có thể mang thai trong tương lai.
Nó có thể được thực hiện theo những cách khác nhau:
- Phẫu thuật mở ổ bụng, trong đó u xơ được loại bỏ thông qua một vết cắt Phẫu thuật mở ở bụng.
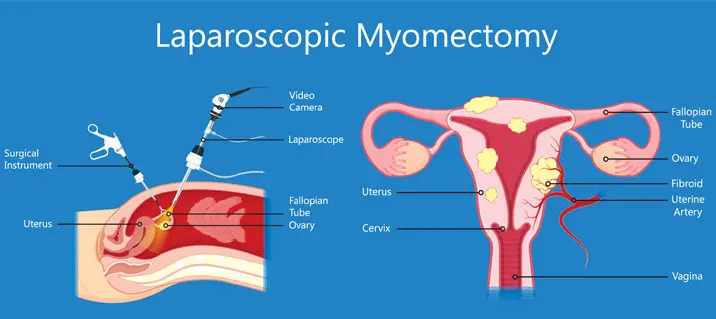
- Phẫu thuật cắt bỏ u xơ nội soi, loại bỏ u xơ thông qua một số vết mổ nhỏ. nó ít xâm lấn hơn so Với Phẫu thuật cắt u xơ qua mở ổ bụng và thời gian phục hồi ngắn hơn.
- Phẫu thuật cắt bỏ u xơ qua nội soi tử cung, còn được biết đến là Phẫu thuật Cắt bóc Hạch Myoma qua Cổ Tử cung (TCRM), sử dụng một phạm vi đặc biệt để loại bỏ u xơ qua âm đạo và cổ tử cung.
Điều trị u xơ nếu bạn không cố gắng thụ thai
Nếu việc mang thai không phải là vấn đề đáng lo ngại hoặc nếu bạn không có ý định thụ thai, bác sĩ phụ khoa có thể đề nghị phương pháp thuyên tắc động mạch tử cung (UAE) hoặc cắt bỏ tử cung.
Các thủ tục này thường không được khuyến khích cho những người muốn thụ thai, đó là lý do tại sao bạn nên nói chuyện chi tiết với bác sĩ để được biết về những rủi ro có thể xảy ra.
Thuyên tắc động mạch tử cung (UAE)
Trong phương pháp thuyên tắc động mạch tử cung (UAE), u xơ bị tiêu diệt bằng cách cắt nguồn cung cấp máu của chúng.
Liệu pháp siêu âm hội tụ hướng dẫn bằng MRI
Liệu pháp siêu âm hội tụ hướng dẫn bằng MRI là một kỹ thuật không phẫu thuật, phá hủy u xơ bằng sóng siêu âm cường độ cao.
Cắt bỏ tử cung
Để chấm dứt các triệu chứng, bạn có thể chọn phẫu thuật cắt bỏ tử cung, trong đó tử cung được cắt bỏ nhưng buồng trứng, nơi chịu trách nhiệm sản xuất hormone sinh sản nữ, được giữ nguyên để bạn không bước vào thời kỳ mãn kinh sớm.
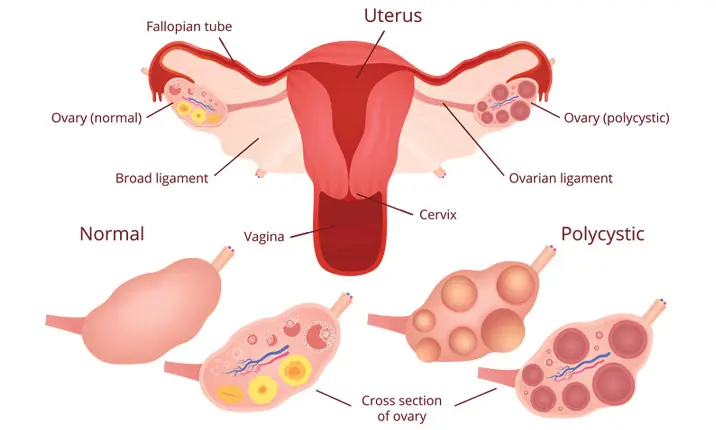
U nang buồng trứng là gì?
Buồng trứng của bạn chịu trách nhiệm sản xuất các hormone điều chỉnh hệ thống sinh sản của bạn.
Buồng trứng cũng giải phóng trứng là trung tâm của chu kỳ rụng trứng. Cũng trong chu kỳ rụng trứng hàng tháng này, một u nang - một túi chứa đầy chất lỏng - trên một hoặc cả hai buồng trứng có thể hình thành.
U nang buồng trứng có thể lành tính hoặc ác tính:
- u nang buồng trứng lành tính bao gồm u nang cơ năng, u nang tuyến, u nang nội mạc tử cung, u nang nhầy và u nang bì. là các u lành nhưng vẫn có thể Hóa ác tính.
- các khối u ác tính bao gồm ung thư buồng trứng biểu mô Hoặc khối u tế bào mầm.
U nang buồng trứng dạng u nang cơ năng thường xảy ra mà không có triệu chứng, khi một trong những nang chịu trách nhiệm giải phóng trứng không mở ra được. Chúng thường tự khỏi trong vòng vài tháng mà bạn không nhận ra.
Bởi vì hầu hết các u nang buồng trứng xảy ra trong chu kỳ rụng trứng nên chúng ít phổ biến hơn ở những phụ nữ đã trải qua thời kỳ mãn kinh.
Các triệu chứng của u nang buồng trứng là gì?
Các triệu chứng và biến chứng phát sinh nếu u nang phát triển lớn bất thường hoặc vỡ.
Những phụ nữ mắc hội chứng buồng trứng đa nang thường thấy có nhiều u nang nhỏ phát triển trên buồng trứng. Đây là nguyên nhân phổ biến gây vô sinh.
Sự khác biệt giữa u nang buồng trứng và u xơ là gì?
Sự khác biệt chính giữa u nang buồng trứng và u xơ tử cung là u nang đôi khi có thể tự biến mất mà không gây ra triệu chứng.
Nếu bạn bị đầy hơi, tức bụng, đau vùng chậu, đau khi giao hợp, hãy tham khảo ý kiến bác sĩ phụ khoa để được chẩn đoán chính xác. Nếu cơn đau đột ngột và dữ dội, đặc biệt nếu kèm theo nôn mửa và sốt, hãy tìm kiếm sự chăm sóc y tế khẩn cấp tại các bệnh viện có chuyên khoa phụ sản hoặc bệnh viện chuyên khoa phụ sản.
U nang buồng trứng được điều trị như thế nào?
Nếu bạn đã được chẩn đoán mắc u nang buồng trứng, bác sĩ phụ khoa có thể áp dụng phương pháp chờ và theo dõi để xem liệu nó có tự khỏi hay không.
Siêu âm vùng chậu
Nếu bác sĩ khuyên bạn nên theo dõi và chờ đợi, tình trạng của bạn sẽ được theo dõi bằng siêu âm vùng chậu định kỳ.
Siêu âm vùng chậu sử dụng sóng âm thanh tần số cao để tạo ra hình ảnh tử cung và buồng trứng của bạn. Điều này sẽ giúp bác sĩ xác nhận sự hiện diện của u nang, vị trí và đặc tính của nó.
Xét nghiệm máu đánh dấu khối u ung thư
Bác sĩ cũng có thể đề nghị thực hiện xét nghiệm máu đánh dấu khối u, được gọi là CA125, để đánh giá nguy cơ ác tính. Xét nghiệm này phát hiện nồng độ kháng nguyên ung thư 125 tăng cao, thường gặp ở phụ nữ mắc bệnh ung thư buồng trứng.
Thuốc tránh thai
Nếu bạn bị u nang buồng trứng tái phát, bạn có thể được kê đơn thuốc tránh thai. Điều này giúp ngăn ngừa sự hình thành các u nang trong tương lai trong quá trình rụng trứng.
Mặc dù điều này sẽ không thu nhỏ u nang hiện có nhưng thuốc tránh thai có thể làm giảm nguy cơ ung thư buồng trứng.
Phẫu thuật nội soi xâm lấn tối thiểu
Nếu u nang là nguyên nhân đáng lo ngại, bác sĩ phụ khoa có thể sử dụng một thủ thuật xâm lấn tối thiểu gọi là phẫu thuật nội soi để kiểm tra tình trạng.
Quy trình này sử dụng một camera nhỏ được đưa vào qua các vết mổ nhỏ có kích thước lỗ khóa ở bụng.
Cắt bỏ u nang buồng trứng
Trong quá trình phẫu thuật nội soi, bác sĩ phụ khoa cũng có thể loại bỏ u nang. Đây được gọi là phẫu thuật cắt bỏ u nang buồng trứng, loại bỏ u nang trong khi vẫn giữ nguyên buồng trứng.
Cắt bỏ buồng trứng
Đối với một số phụ nữ, phẫu thuật cắt bỏ buồng trứng (cắt bỏ một hoặc cả hai buồng trứng) có thể cần thiết nếu buồng trứng không thể bảo tồn được.
Có một số phương pháp có thể được chọn lựa thực hiện:
- cắt bỏ một bên buồng trứng.
- cắt bỏ hai bên buồng trứng.
- cắt bỏ một bên buồng trứng và ống dẫn trứng dẫn trứng từ buồng trứng đến tử cung.
- cắt bỏ hai bên buồng trứng để loại bỏ cả buồng trứng và ống dẫn trứng.
- Cắt bỏ toàn bộ tử cung kèm theo cắt bỏ ống dẫn trứng và buồng trứng 2 bên hoặc 1 bên.
Nếu cả hai buồng trứng bị cắt bỏ, bạn sẽ không thể sản xuất trứng được nữa và thời kỳ mãn kinh sẽ bắt đầu ngay lập tức.
Chẩn đoán sớm u nang buồng trứng và u xơ tử cung
Chẩn đoán và điều trị sớm là chìa khóa để điều trị thành công cả u nang buồng trứng và u xơ tử cung.
U nang buồng trứng và u xơ tử cung ban đầu có thể phát triển mà không có triệu chứng. Tuy nhiên, khi chúng tăng kích thước hoặc số lượng, các triệu chứng có nhiều khả năng xuất hiện hơn và tốt nhất bạn nên tìm tư vấn y tế càng sớm càng tốt vì việc chẩn đoán sớm thường cải thiện kết quả điều trị.
Hãy đặt lịch hẹn với bác sĩ phụ khoa nếu bạn nhận thấy bất kỳ triệu chứng đáng lo ngại nào.
Fibroids and Cysts. Retrieved 12/5/2020 from https://mtalvernia.sg/education/fibroids-and-cysts/
Uterine Fibroids, Endometrial Polyps and Ovarian Cysts. Retrieved 12/5/2020 from https://rmob.coloradowomenshealth.com/health/fibroids-polyps-cysts
Ovarian Cysts and Uterine Fibroids - Symptoms and Treatment. Retrieved 12/5/2020 from https://www.brighamandwomens.org/obgyn/infertility-reproductive-surgery/cysts-and-fibroids
Uterine Fibroids, Endometrial Polyps and Ovarian Cysts. Retrieved 12/5/2020 from https://rmob.coloradowomenshealth.com/health/fibroids-polyps-cysts
Ovarian Cysts and Uterine Fibroids - Symptoms and Treatment. Retrieved 12/5/2020 from https://www.brighamandwomens.org/obgyn/infertility-reproductive-surgery/cysts-and-fibroids